Tim Jackson

Lyudmila’s Cancer
We were planning a New Year holiday with friends in Copenhagen when Lyudmila announced she had a pain in her left breast. There was no lump or visible mark, but it felt a bit firmer in the sore area. She went to see the doctor straight away. As she was 45 and her once clockwork periods had become irregular, it was put down to menopausal hormone changes.
In early 1997 she was quite sore and the left side became a sexual no-go area. She saw the doctor several times, who eventually pronounced it to be mastitis. She would just have to put up with it until it went away, probably with the menopause. We were not satisfied and I suggested she see another partner at the Health Centre, but she wanted her regular female doctor for this "woman's" complaint.
She has always tended toward mood swings and depression, I used to be able to predict her periods from her mood. As the year progressed the depressions got more prolonged, and more frequent. I put this down to the small but persistent nagging pain from her breast.
The breast became swollen and misshapen, visibly so through a summer dress. The doctor suggested she go up a bra size, saying "Lyudmila, you do not have cancer!" to her anxious queries.
It was August, during the doctor's holidays when nipple discharge started. She said she smelled like a sheep. Another appointment, this time with another female doctor led to mammogram, mastectomy and chemotherapy and radiotherapy. They took a 7cm diffuse tumour and 14 affected lymph nodes from her, and pronounced her clear.
With the mastectomy the depression lifted like a cloud. She still had discomfort from the surgery and chemo, so it had to have been the cancer itself which gave her such a bad time.
It was about a year later when I spotted a sideboard in a friends house which looked out of place, but would suit our house perfectly. They needed more space, so we bought it and took it home in our van. I persuaded Lyudmila against her better judgement to help me move it into the house. I had it out of the van and could lift the thing alone but couldn't manoeuvre it, and I didn't want to get a neighbour out late at night for such a little thing. A few days later she complained of back pain around the bottom of her shoulder blades. Well I felt like a shit, but these things happen. We massaged it, but it didn't help much. The oncologist and the GP said she should wait, back pains usually heal themselves after about 6 weeks, and declined to do a bone scan. "What if it is secondary cancer?" We had talked and read about what might happen. "No, cancer pain is much worse than that. Bone tumour patients need painkillers and sweat from the pain." I thought "Yes, but could this be how it starts? It can‘t just appear, full blown, there has to be a progression" but Lyudmila wanted to run this conversation so I kept it to myself. Later I learnt that taking the rough side of her tongue was better than leaving questions unasked..
After three months of fruitless physiotherapy she saw an orthopaedic surgeon who immediately ordered a bone scan and found a spinal tumour. This was duly zapped with radiotherapy. She was given a stack of drugs, morphine to dull the pain, volterol ( a ibprofen non-steroid anti-inflammatory drug or NSAID) to reduce the inflammation that caused the pain, Cimetidine acid suppressant and Domperidone anti-emetic to combat the (rather contrary) inflammatory side effects of NSAIDs on the stomach.
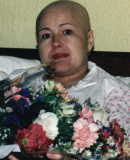 The pain persisted for a couple of months then slowly faded. Almost as soon as it was gone another one started, higher up. This time no trouble getting a bone scan, but when the results came the junior doctor who saw us was very evasive and hid the report like a schoolgirl afraid of her classmates copying. Multiple tumours all down the spine and in the ribs. More radiotherapy, and chemotherapy: Epirubicin and Taxol on a clinical trial. There goes the hair.
The pain persisted for a couple of months then slowly faded. Almost as soon as it was gone another one started, higher up. This time no trouble getting a bone scan, but when the results came the junior doctor who saw us was very evasive and hid the report like a schoolgirl afraid of her classmates copying. Multiple tumours all down the spine and in the ribs. More radiotherapy, and chemotherapy: Epirubicin and Taxol on a clinical trial. There goes the hair.
Increasing pain meant increasing morphine doses until the side effects set in. She became very lethargic, sleeping over 18 hours a day and being confused when she was awake, she twitched all the time, even in her sleep, her breath, urine and sweat began to smell of the drug metabolites. Constipation was a problem, and resulted in haemorrhoids. It turned out that the drug stack should have included laxatives to combat this side effect of morphine. Although a regular dose solved the problem, she tended to stop taking the laxatives once her bowels were normal, leading to an oscillation between constipation and diahorrea.
The hospital pain control team took a hand and changed her analgesic to Fentanyl patches. Fentanyl needs about 150 times less drug to achieve the same effect, so there are less metabolites and less side effects. The skin patches also mean a more even dose of drug, and no stomach stress.
Now the problems began to overlap. More shots of radiotherapy. On one occasion, a new tumour developed while waiting for a slot on the radiotherapy machine to treat the previous one. Fortunately it doesn't take long to program in extra targets, and they were able to shoot both.
The bad news was the collateral damage. She got sick, her temperature shot up and her haemoglobin count shot down all in quick succession. It all came to a head on New Year’s Eve, and we made what was probably the first emergency call to the Christie Hospital of the millennium. Probably irradiating her lumbar region had inflamed her stomach, the inflammation was sustained by the NSAID she was taking for her bone disease. The inflammation would haemorrhage, causing the anaemia.
Blood transfusions, antibiotics and juggling medication took about two months to get this right, but by then she was on the final slope. To keep the bone pain under control and the analgesic dose low enough to stay awake she still needed NSAID. The solution was to use Volterol suppositories, intended for children. Once she stopped being sick she still couldn't eat, and the symptoms we had seen with morphine overdose began to reappear. It became clear that the cancer was now rampant in her soft tissues.
The 'overdose' problems were attributed to liver tumours, accumulating rather than disposing of metabolites. Reducing the Fentanyl helped, but there was clearly another problem. The lack of appetite was attributed to mechanical pressure of tumours on her digestive system. No one quite explained the lethargy and confusion. Calcium levels were suspected, but remained irritatingly normal. Eye examination showed no sign of brain pressures, but I feel something must have been going on in there too.
At this stage it was clear that she would die soon, and the medical activity centred around keeping her comfortable. Any further attempt to prolong her life could only prolong her suffering. She became incontinent and was totally confused on the rare occasions when she woke.
I had made a bed in the back of our van for transporting her to and from hospital when she could not take sitting. This worked well until she was no longer able to get downstairs to get in the van. From then we had to use the ambulance service. It seemed odd that in order to help bringing her downstairs the ambulance had to make the 30-mile trip to the hospital, which I was making anyway, but in fact the ambulance was often taking several passengers.
After twice coming to her room and finding her on the floor, I began to be afraid to sleep in case something happened. The District Nurses were visiting twice a day to help with her medication and hygiene, but I realised I could no longer manage her on my own. The doctors agreed and arranged for her to move to the Hospice in Blackburn about seven miles away. There is one closer, but it is heavily sponsored by the GP who originally misdiagnosed her cancer, and has photos of said lady on the walls. I felt that is would be inconsiderate in the extreme to let her die in front of the image of the person who in her mind was her killer.
She went there by ambulance, I followed and caught up with her at the Hospice reception. She smiled to see me, for the last time. Once she was settled in, she fell asleep. The consultant there changed her analgesic to a Morphine pump, and put a catheter in to empty her bladder continuously. She did not wake again, and after two days, her breathing became irregular and stopped.
 The pain persisted for a couple of months then slowly faded. Almost as soon as it was gone another one started, higher up. This time no trouble getting a bone scan, but when the results came the junior doctor who saw us was very evasive and hid the report like a schoolgirl afraid of her classmates copying. Multiple tumours all down the spine and in the ribs. More radiotherapy, and chemotherapy: Epirubicin and Taxol on a clinical trial. There goes the hair.
The pain persisted for a couple of months then slowly faded. Almost as soon as it was gone another one started, higher up. This time no trouble getting a bone scan, but when the results came the junior doctor who saw us was very evasive and hid the report like a schoolgirl afraid of her classmates copying. Multiple tumours all down the spine and in the ribs. More radiotherapy, and chemotherapy: Epirubicin and Taxol on a clinical trial. There goes the hair.
